New Tech Improving Outcomes for Bladder Cancer, but Barriers to Access Remain
Research and Innovations The most expensive cancer to treat is also the one with the highest recurrence rates. Find out how new developments are making it easier for doctors to diagnose and how technology is allowing for more equal access.
In many ways, bladder cancer stands out from other cancers, much like the red lemon stands out in Bladder Cancer Canada’s iconic “See Red? See Your Doctor” campaign. It is one of the most commonly diagnosed cancers, but also one of the most treatable. It has one of the highest recurrence rates, at 60 percent to 70 percent. And, it is the single most expensive cancer to treat.
Reducing recurrence can reduce cost and surgeries
For decades, treatments for bladder cancer have stayed essentially the same, with little available to reduce the recurrence or the cost. But now, new developments are starting to change the outlook for the future.
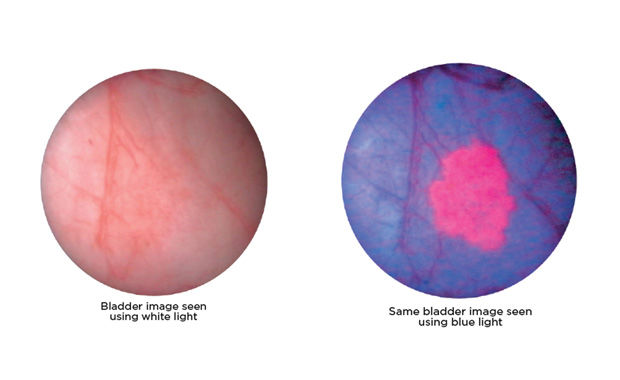
One of these new developments is blue light cystoscopy (BLC), which causes tumours in the bladder to distinctly fluoresce, allowing doctors to detect even small and flat tumours at the time of surgery. “In bladder cancer, you may see one tumour with the regular white light, but there are commonly other smaller tumours nearby that you may not see,” explains Dr. Peter Black, a Urologic Oncologist at Vancouver General Hospital and Professor of Urologic Sciences at the University of British Columbia. “BLC can reduce the number of trips to the operating room and help avoid additional surgeries. That can be a huge help for the patient’s recovery.”
“You feel like you’re pinned down”
This sentiment is very much shared by Richard Hustler, a bladder cancer patient who has just had his second surgery in three years. “I have to start all over again with my treatment,” Richard says. “I think I’m doomed to regular visits with my urologist for the rest of my life, but if I can avoid any more surgeries that will be really good. It really makes you feel like you’re pinned down by it, when you’re always scheduled for one treatment or another.”
Although BLC has been approved for use in Canada since 2015, it is still not widely available. “A lot of new technologies like this one can be very budget dependent for hospitals,” says Stephen Wilson of Bladder Cancer Canada’s Board of Directors.
Sometimes, however, looking strictly at up-front cost can be misleading, as additional spending on treatment can be offset by reduced costs on follow-up. Analyses have shown that BLC pays for itself by lowering the rate of recurrence. This is important because much of what makes bladder cancer so expensive to the system is in the surveillance after treatment.
Of course, as with any new technology, adoption can’t happen all at once. But when that technology improves outcomes for the roughly 9,000 Canadians who are newly diagnosed with bladder cancer every year, and does so without increasing costs, equal access becomes a necessity.
