Brightening The Future For Children With Brain Cancer
Research and Innovations Meet seven-year-old Jax, a pediatric brain tumour survivor whose tragic story is all too common. Groundbreaking brain cancer research hopes to change that.
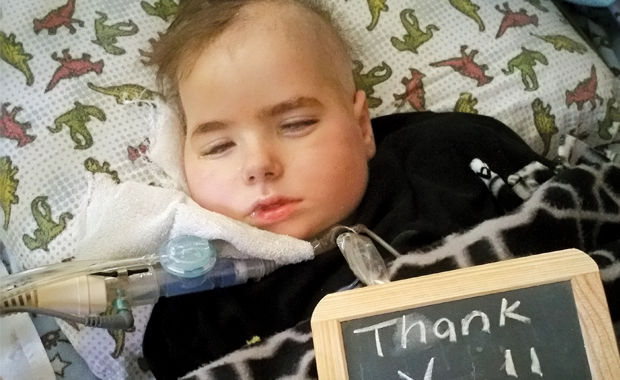
When some people look at seven-year-old Jaxson, they see a brain tumour survivor who is now unable to breathe, eat, or stand on his own, but Candace Breynaert simply sees her son.
Jax was just a toddler when he started vomiting profusely and losing developmental milestones, to the point that he could barely lift his head off the floor. His family decided enough was enough and took him to the hospital, where the tiny two-year-old had a seizure in his mother’s arms. After extensive scans, physicians found out why. Jax had a medulloblastoma tumour, the most common form of childhood brain cancer.
“It was heart wrenching,” says Breynaert. Jax endured surgery and high-dose chemotherapy, and was eventually declared tumour-free — but eight months later, his cancer returned.
“Hearing it the second time, that was the worst feeling,” says Breynaert, who left her job to care for Jax full-time. “You’re not left with many options because you’ve pretty much exhausted them the first time around.”
Jax’s story is tragic, but not uncommon, says Susan Marshall, CEO of Brain Tumour Foundation of Canada, who lost her son to medulloblastoma.
Every day 27 Canadians learn they have a brain tumour, a diagnosis that is particularly challenging for children. Brain tumours are the leading cause of solid cancer-related death in children, and the 60 percent of children who do survive often live with long-term side effects.
“Your brain is so central to your life and your quality of life that there is a sense of urgency around this,” says Marshall. “We really need to do something better for these patients and their families.”
Changing perspectives
When brain cancer patients are diagnosed, physicians look at the makeup of their tumour to determine the best course of therapy. If the tumours return after treatment, medical teams typically decide the next steps based on what they knew about the tumours at diagnosis. However, new research has found flaws in this approach.
“For a long time people thought of cancer as a static thing that wouldn’t change, like a picture of an old relative that hung over the fireplace for 200 years and just stayed the sam.”
According to a study published in Nature, the genetic makeup of tumours in children with medulloblastoma is vastly different at diagnosis than at recurrence.
“For a long time people thought of cancer as a static thing that wouldn’t change, like a picture of an old relative that hung over the fireplace for 200 years and just stayed the same,” says Dr. Michael Taylor, a neurosurgeon at The Hospital for Sick Children and co-supervisor of the study featured in Nature. “Now we know that cancer is more like a movie — it changes over time.”
With these findings, Dr. Taylor says that when tumours recur, physicians can now provide targeted treatments that are more effective and less toxic, hopefully improving outcomes for brain cancer patients.
“The way things were before, there was only a 1 in 20 chance of anything working,” says Dr. Taylor. “We want to make it so there’s a 20 in 20 chance.”
A brighter future
Marshall says brain tumour research like Dr. Taylor’s study is essential for providing some hope to patients facing unthinkable odds.
“There have been major advancements for some cancers, but not for brain cancer,” says Marshall. “We need to focus on it to make a difference.”
Improving brain cancer treatments does make a difference for patients like Jax.
“Knowing that we have options is everything to us,” says Breynaert. “Options in our world are huge, because we don’t get them very often.”



.jpg)